This week marks my ten year Crohniversary – a decade of living with a diagnosis of Crohn’s disease. It’s hard to conceive where those ten years have gone, as I can quite easy close my eyes to find myself back as that 14-year old terrified at the prospect of having to live with this tortuous disease for the rest of my life.
How it all began
Like so many other people, my battle with Crohn’s disease (a form of inflammatory bowel disease, IBD) started long before I received that diagnosis during the last week of April 2008. In reality, I had been symptomatic from 2006, towards the end of my first year of high school. The journey to get referred to the paediatric gastroenterology team was difficult – with my mum often feeling neurotic in fighting for me, with little success. Time after time, I was told it was ‘only’ constipation – after which I’d be given sachets of
Movicol to take – which in hindsight, just irritated the situation further.
You would think that if you were already under the care of a specialist team at the hospital (as I was for my juvenile idiopathic arthritis), that the process of joining up symptom patterns and investigating them would have been much more efficient – but unfortunately, that wasn’t the case. Even after seeing the gastroenterology team, there didn’t seem to be much cause for concern – with constipation again labelled as the ‘reason’ for the symptoms. It had never been discussed with me that arthritis and IBD could be linked, so why on earth would I have ever questioned that? I didn’t have the foggiest clue about IBD – and it was long before the days of online support groups and places where I could find that kind of information as a teenager. Though to be honest, I don’t think I would have had the confidence to question and suggest things to the healthcare professionals – I just felt as though nobody was listening or cared about how I was feeling.

I was an atypical case too (as per usual), which didn’t help the speed of diagnosis. Given my active joint inflammation, my inflammatory markers were already elevated, and I had recently been on intermittent courses of
steroids – which as we’ve seen in the news recently thanks to
Dynamo, can cause some rather unpleasant side effects – including weight gain and ‘moon face’. Though looking back on photos now, I had clearly lost weight in the months leading up to my diagnosis. The other cause for this delay was quite simply because nobody seemed to listen to me, or understand how much pain and discomfort I was in. At several points, I had begun to think to myself that it was ‘all in my head’ – which only inflamed my anxiety, which I bottled up inside. I felt guilty for wanting these symptoms to be labelled as a disease – which I shouldn’t have felt guilty for at all. I just wanted answers as to why my body felt as though it was falling apart.
After what seemed like months of waiting for paint to dry, I was seen again by a paediatric gastroenterologist, who said it was very unlikely to be Crohn’s disease or ulcerative colitis, but for ‘peace of mind’, he would arrange a
gastroscopy and a
colonoscopy. This was probably the first time that I had heard of ‘Crohn’s disease’ or ‘ulcerative colitis’, and still didn’t have much idea what it was. I remember sitting in the waiting room area at
Booth Hall Children’s Hospital after this appointment while I waited for blood tests, and I read the littered notice board posters in more detail – which was evidently not tailored for children and young people! I remember seeing people with this ‘Crohn’s disease’ and there was talk about colostomies, bowel cancer, and various other frightening things, which gave me this horrible, sinking feeling about what could lie ahead.
Nearing a diagnosis
Some time later, I had finally received a date to be admitted to Ward 14 at Booth Hall Children’s Hospital. My band was placed on my arm, the cannula was inserted, and I was ready to go… not to mention the preceding 24 hour fasting period and the consumption of several litres of the most vile bowel preparation liquid – which was (and remains) far worse than having the procedure itself! I remember leaving my parents in the side room that I was in, as I was wheeled down to theatre. Thankfully, I was placed under general anaesthetic for the procedures, and before I knew it, I was in recovery. Once I was taken back to the ward, I had time to sleep – but then, the doctor came into the room, not looking his usual cheery self, which automatically set off alarm bells in my head.
Ten years on, I can picture the situation, and I can hear the echoes of what he said. Having sat on the corner of my bed, he looked directly to me, not my parents, and said…
I am so, so, sorry Simon. I never realised how bad you really were.”
As things unfolded, he went on to tell me that I had Crohn’s disease. From my oesophagus right the way through to the ‘other end’, there were ulcers spreading through the surface and wall of my inflammed gastrointestinal tract. Swift action needed to be taken, and I was presented with drugs and options left, right and centre – which was all a little too much to take in. Firstly, I would have to be taken off
etanercept, which I was injecting twice a week to help manage my arthritis, since this had been ‘masking’ the Crohn’s disease. The next option would have to be
infliximab, but discussions would need to take place with the rheumatology team. I was placed onto steroids yet again, and I was prescribed a drug called
mesalazine. To help with acid reflux, I was prescribed
omeprazole and
domperidone was given to help me with the nausea and vomiting that I had been experiencing for quite some time. He also suggested that to help rest my gastrointestinal tract, that I should be placed on a polymeric diet, which is a nutritionally complete liquid diet (in the form of
Ensure Plus shakes) which can be easily digested, and contain all the necessary vitamins that you need. I would need to be on this diet exclusively for 8 weeks, with only plain water permitted. He said that many people struggle to stick to this diet, but if you can, it can help to set you off on the right course into remission. I was that desperate to feel better, so I just said yes, I’ll give it a go. Little did I know that I would need to drink eight of these shakes a day – the first couple weren’t too bad, but it was so difficult to get the rest down without heaving or vomiting – and I certainly think it put me off milk for life!
I remember the first night I spent in hospital after being diagnosed – my mum and dad went home at about 8 pm, and shortly after, the lights went out in the ward. I found myself lay in bed in the side ward cubicle – alone. All of a sudden, the tears came from nowhere, and I cried myself to sleep, worrying about what was going to happen to me. My biggest fear was that I would need a
colostomy bag; it was one of the thoughts that I could just not get out of my head. It terrified me, and I was ashamed of sharing that fear with anyone – including my family.
I spent over a week in hospital – in which time, I should have been completing my Year 9 SATs in school. Certain members in school wanted me to sit these tests at the hospital – days after receiving my diagnosis, and it was certainly an external stress factor that I did not need at that time. Thanks to my parents and staff at the hospital, school agreed to take my predicted levels as an indicator. Once home, I had to become accustomed to my ‘new’ life with both arthritis and Crohn’s disease, while manoeuvring the boxes of Ensure Plus shakes which had been delivered. I also had to start quashing my phobia of tablets, which had previously been brought on because of my unpleasant experience from
methotrexate. Within a few weeks, I was determined to get back to ‘normal’ and return to school, which I did. Unfortunately, I hadn’t prepared myself – physically or mentally, for that return, which just felt completely overwhelming. I was anxious, nervous and ashamed of myself – not to mention being terrified of people laughing at me, or finding myself having an accident if I couldn’t get to the toilet in time.
Thankfully, school were much more understanding this time around and helped to arrange home tutoring for me through the local authority, to give me some extra time to come to terms with my diagnosis, and build up my strength and resilience ahead of moving into Year 10. I came back to school just before the end of the school year, which was a better way to ease myself back into things, before the summer holidays – during which, I began to change treatments onto infliximab… which didn’t work! Some months and more steroids later, I was switched again onto
adalimumab, my third biologic treatment, which *touch wood* has been on the whole effective in managing both my arthritis and Crohn’s disease. I remain on it today, some 10 years later.
 Learning to live with change
Learning to live with change
Over the years, I have certainly learned to live with Crohn’s disease, and my understanding of the condition has greatly increased. I’ve learned to predict the signs of when a flare may be happening, and what I need to do be proactive in managing the condition. As may be expected, one of the biggest triggers for me is stress – as is the case for so many others, and so it was always a worry around coursework and exam time that my Crohn’s disease would flare – as it usually did. I had noticed that my symptoms worsened when I was stressed, and this made me even more anxious just thinking about getting stressed – and so the vicious cycle just kept on festering. At times, I did question whether it was worth putting myself under all of this pressure, to achieve the grades I wanted. As many of you will know, I am a perfectionist, and so anything below an A to A* grade at GCSE was a failure to me – silly I know, but we can’t change our personalities! In hindsight, I’m so glad that I stuck with it all, gaining 16 GCSEs and 3 A-Levels, before starting my undergraduate degree at The University of Manchester in Biomedical Sciences in 2012.
As part of my degree, I spent a year working in a medical communications company. This was my first experience of working full-time, in an office environment, and while I was excited for the new opportunities I would experience, I was also anxious about how I would cope in working full-time and managing my health. Luckily, my employers were fantastic, and were extremely flexible. I was able to work at home when I needed to, and I could move my working hours around my personal needs, which is the absolute ideal for people like me with conditions such as Crohn’s disease.
After a year of working, I returned to university to complete the final year of my degree and, in 2016, I graduated with a first class honours degree! While I loved so many aspects of my degree, the amount of stress I was under was something else, particularly around exam time and particularly during my final year. The stress unfortunately did impact on my health and without the support that I had, this would have undoubtedly have been much worse. This is why I cannot emphasise enough about the importance of ensuring that the right support is in place at university from the earliest opportunity, in order to eliminate as much unnecessary stress as you can. We must all speak up for ourselves, to ensure that we are supported in the way that we should be. I know it is easier said than done, but it really will pay off in the long run. Looking back to my younger years, I certainly wasn’t as vocal as I am now, and didn’t stick up enough for myself, or fight for what I really needed – usually out of concern of offending or being a burden to others.
Ten years on… the journey never ends
Ironically, ten years on, I find myself back and forward between the gastroenterology team as an adult, as we get to the bottom (pardon the pun) of what’s happening this time around… Don’t worry, I hear those kind of jokes all of the time – you’ve got to laugh! While it’s still taking time to find out whether it’s a flare, a complication, something related to Crohn’s disease, or something else completely, what has changed is that I’m very much leading and steering the conversations – I’m very much in the driving seat, asking those awkward questions, and probing for answers with suggested approaches and things to rule out, simply because I’m informed, and I’m empowered.
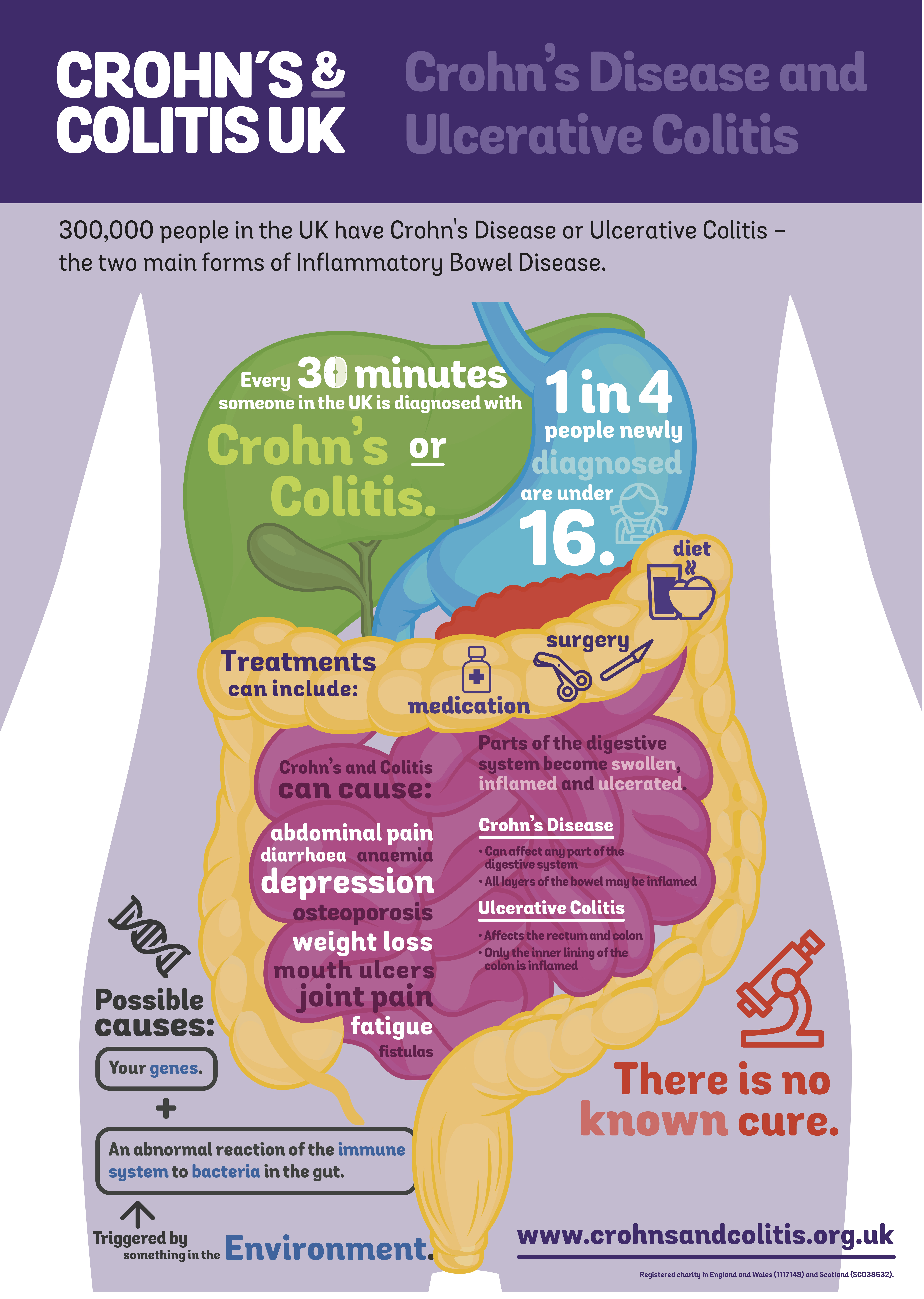
What you can never really prepare for is the burden that comes with some of the symptoms of Crohn’s disease. We’re so bad as a nation at talking about so many things related to our bodies – especially toilet talk! This only aggravates how people with bowel problems feel. Can you imagine trying to walk a short distance, but then you suddenly have to stop and stand still, because you are terrified of having an accident? It’s been happening to me more and more in the last few months – and it really has an effect on what I do. Imagine standing up on a jam-packed train into Manchester at 7 am in the morning, while it feels as though your guts are about to burst – the pain is ripping through your body, and you can’t even get to the main part of the carriage to ask for a seat because you’re wedged up against the door. It’s terrible – and something I dread on a daily basis, despite looking completely fine – and attempting to fill my life with all of the things that I love to do. I came across the below graphic earlier today, and I was struck by how well it portrays what Crohn’s disease feels like, and more importantly, demonstrates what’s happening inside the bodies of so many people who, like I, struggle to convince others to the extent of what’s really happening to our bodies.
 Source: B. R. Keller
Source: B. R. Keller
Last week, I spent a considerable amount of time at Manchester Royal Infirmary, while I had a colonoscopy, an MRI scan of my small bowel, and an appointment with the gastroenterology nurse. Unfortunately, the colonoscopy was unsuccessful, as after an hour, my doctor was unable to progress through my bowel, because it was collapsing around the scope and obstructing his view. The sedation had well and truly worn off, and despite moving around myself, and having the nurses pushing my abdomen left, right and centre (I’ve got the bruises to prove it), it was just not working. So I’ll need to go back in (and yes, I’ll need to drink another few litres of bowel preparation, yuck) for a different type of colonoscopy – most likely a balloon colonoscopy. The MRI was relatively straight forward, and I’ve still to receive the results from this. I then was in the nurse clinic last Wednesday, and I have to say that the IBD nurses at Manchester Royal Infirmary are really lovely. We had a really productive conversation, and while we wait for the test results, she very much listened to the problems that I’m having has arranged even more tests and referrals, to help speed up the process of helping me to find some answers as to what’s going on at the moment, so that I can hopefully get back on track.
With
World IBD around the corner, I want to remind my friends, colleagues and followers of the impact and difficulties that Crohn’s disease (and ulcerative colitis) can impose on the lives of those with the condition, as well as their family and friends. Simple acts of kindness, such as not judging somebody for using a disabled toilet, or asking to take your seat on the train, can make all the difference, because you never know whether those individuals have IBD, or other invisible conditions which makes things extra challenging for them. The world would be a much happier and inclusive place if people could just go about their daily lives without fear of judgment or criticism – and it remains the responsibility of us all to help make this a reality.

Never take things for granted
One thing that I’ve learned to appreciate over the years is that none of us should take anything for granted. Despite obvious frustrations, I feel incredibly lucky to have access to treatment and care, which is a privilege many people around the world don’t have. However, the future remains uncertain – it does for us all, but particularly for those of us living with chronic, long-term conditions. So if you see me making the most of my travels abroad when I’m out speaking at an event, or if you see me out with friends enjoying a cocktail or two – you can be certain that I’m having a brilliant time, but it’s certainly not because I have charmed, perfect life. It’s because I know what it’s like to be unable to do things that you desperately want to do, and because I know there may be a time when I am no longer able to do some of those things… so I seize every opportunity I have to meet new people, experience new cultures, and embrace the world around me, because…
nothing is more expensive than a missed opportunity.”
 I was an atypical case too (as per usual), which didn’t help the speed of diagnosis. Given my active joint inflammation, my inflammatory markers were already elevated, and I had recently been on intermittent courses of steroids – which as we’ve seen in the news recently thanks to Dynamo, can cause some rather unpleasant side effects – including weight gain and ‘moon face’. Though looking back on photos now, I had clearly lost weight in the months leading up to my diagnosis. The other cause for this delay was quite simply because nobody seemed to listen to me, or understand how much pain and discomfort I was in. At several points, I had begun to think to myself that it was ‘all in my head’ – which only inflamed my anxiety, which I bottled up inside. I felt guilty for wanting these symptoms to be labelled as a disease – which I shouldn’t have felt guilty for at all. I just wanted answers as to why my body felt as though it was falling apart.
After what seemed like months of waiting for paint to dry, I was seen again by a paediatric gastroenterologist, who said it was very unlikely to be Crohn’s disease or ulcerative colitis, but for ‘peace of mind’, he would arrange a gastroscopy and a colonoscopy. This was probably the first time that I had heard of ‘Crohn’s disease’ or ‘ulcerative colitis’, and still didn’t have much idea what it was. I remember sitting in the waiting room area at Booth Hall Children’s Hospital after this appointment while I waited for blood tests, and I read the littered notice board posters in more detail – which was evidently not tailored for children and young people! I remember seeing people with this ‘Crohn’s disease’ and there was talk about colostomies, bowel cancer, and various other frightening things, which gave me this horrible, sinking feeling about what could lie ahead.
I was an atypical case too (as per usual), which didn’t help the speed of diagnosis. Given my active joint inflammation, my inflammatory markers were already elevated, and I had recently been on intermittent courses of steroids – which as we’ve seen in the news recently thanks to Dynamo, can cause some rather unpleasant side effects – including weight gain and ‘moon face’. Though looking back on photos now, I had clearly lost weight in the months leading up to my diagnosis. The other cause for this delay was quite simply because nobody seemed to listen to me, or understand how much pain and discomfort I was in. At several points, I had begun to think to myself that it was ‘all in my head’ – which only inflamed my anxiety, which I bottled up inside. I felt guilty for wanting these symptoms to be labelled as a disease – which I shouldn’t have felt guilty for at all. I just wanted answers as to why my body felt as though it was falling apart.
After what seemed like months of waiting for paint to dry, I was seen again by a paediatric gastroenterologist, who said it was very unlikely to be Crohn’s disease or ulcerative colitis, but for ‘peace of mind’, he would arrange a gastroscopy and a colonoscopy. This was probably the first time that I had heard of ‘Crohn’s disease’ or ‘ulcerative colitis’, and still didn’t have much idea what it was. I remember sitting in the waiting room area at Booth Hall Children’s Hospital after this appointment while I waited for blood tests, and I read the littered notice board posters in more detail – which was evidently not tailored for children and young people! I remember seeing people with this ‘Crohn’s disease’ and there was talk about colostomies, bowel cancer, and various other frightening things, which gave me this horrible, sinking feeling about what could lie ahead.

 Learning to live with change
Learning to live with change Source: B. R. Keller
Last week, I spent a considerable amount of time at Manchester Royal Infirmary, while I had a colonoscopy, an MRI scan of my small bowel, and an appointment with the gastroenterology nurse. Unfortunately, the colonoscopy was unsuccessful, as after an hour, my doctor was unable to progress through my bowel, because it was collapsing around the scope and obstructing his view. The sedation had well and truly worn off, and despite moving around myself, and having the nurses pushing my abdomen left, right and centre (I’ve got the bruises to prove it), it was just not working. So I’ll need to go back in (and yes, I’ll need to drink another few litres of bowel preparation, yuck) for a different type of colonoscopy – most likely a balloon colonoscopy. The MRI was relatively straight forward, and I’ve still to receive the results from this. I then was in the nurse clinic last Wednesday, and I have to say that the IBD nurses at Manchester Royal Infirmary are really lovely. We had a really productive conversation, and while we wait for the test results, she very much listened to the problems that I’m having has arranged even more tests and referrals, to help speed up the process of helping me to find some answers as to what’s going on at the moment, so that I can hopefully get back on track.
With World IBD around the corner, I want to remind my friends, colleagues and followers of the impact and difficulties that Crohn’s disease (and ulcerative colitis) can impose on the lives of those with the condition, as well as their family and friends. Simple acts of kindness, such as not judging somebody for using a disabled toilet, or asking to take your seat on the train, can make all the difference, because you never know whether those individuals have IBD, or other invisible conditions which makes things extra challenging for them. The world would be a much happier and inclusive place if people could just go about their daily lives without fear of judgment or criticism – and it remains the responsibility of us all to help make this a reality.
Source: B. R. Keller
Last week, I spent a considerable amount of time at Manchester Royal Infirmary, while I had a colonoscopy, an MRI scan of my small bowel, and an appointment with the gastroenterology nurse. Unfortunately, the colonoscopy was unsuccessful, as after an hour, my doctor was unable to progress through my bowel, because it was collapsing around the scope and obstructing his view. The sedation had well and truly worn off, and despite moving around myself, and having the nurses pushing my abdomen left, right and centre (I’ve got the bruises to prove it), it was just not working. So I’ll need to go back in (and yes, I’ll need to drink another few litres of bowel preparation, yuck) for a different type of colonoscopy – most likely a balloon colonoscopy. The MRI was relatively straight forward, and I’ve still to receive the results from this. I then was in the nurse clinic last Wednesday, and I have to say that the IBD nurses at Manchester Royal Infirmary are really lovely. We had a really productive conversation, and while we wait for the test results, she very much listened to the problems that I’m having has arranged even more tests and referrals, to help speed up the process of helping me to find some answers as to what’s going on at the moment, so that I can hopefully get back on track.
With World IBD around the corner, I want to remind my friends, colleagues and followers of the impact and difficulties that Crohn’s disease (and ulcerative colitis) can impose on the lives of those with the condition, as well as their family and friends. Simple acts of kindness, such as not judging somebody for using a disabled toilet, or asking to take your seat on the train, can make all the difference, because you never know whether those individuals have IBD, or other invisible conditions which makes things extra challenging for them. The world would be a much happier and inclusive place if people could just go about their daily lives without fear of judgment or criticism – and it remains the responsibility of us all to help make this a reality.


