Do your hands, fingers or toes ever look white, blue or purple? Scleroderma & Raynaud’s UK (SRUK) estimate that 1 in 6 people in the UK live with Raynaud’s phenomenon, a condition that affects the blood supply to certain parts of the body – usually the fingers and toes. February is Raynaud’s awareness month, so we’re all doing our bit to help raise awareness of this surprisingly common condition.

In people who have
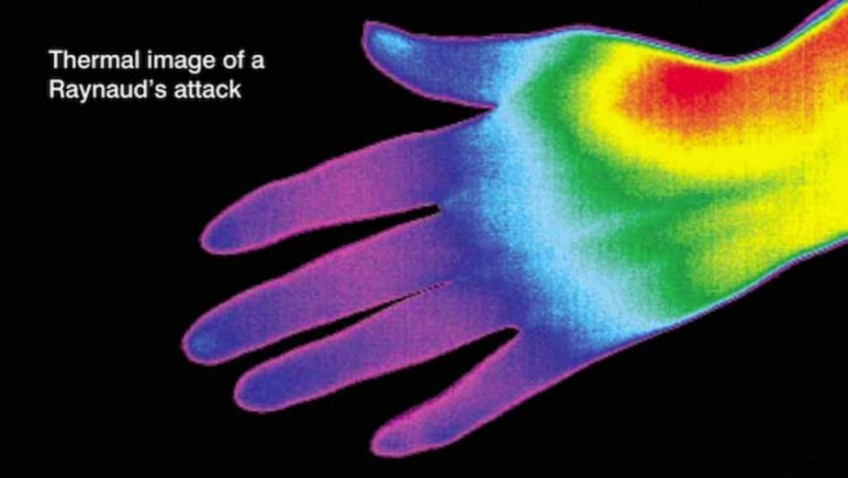
Raynaud’s, the small blood vessels in the extremities such as the hands, feet, fingers or toes are over-sensitive to even the slightest changes in temperature, the cold and sometimes stress. This causes a Raynaud’s attack where the fingers sometimes change colour, but not always, from white, to blue, to red.
A Raynaud’s attack can be an uncomfortable, and possibly painful, process. It can also make everyday tasks, like buttoning a jacket or unzipping a purse, very difficult. Raynaud’s symptoms generally affect the fingers and toes, but all extremities can be involved, including the hands, feet, ears, nose, lips, tongue and nipples.
Symptoms of Raynaud’s include:
- Cold extremities, for example, cold fingers and toes;
- Colour changes in your skin in response to changes in temperature or stress;
- Colour changes from white, to blue/purple and then red;
- Numbness, tingling or pain in the affected area;
- Stinging or throbbing pain upon warming or stress relief.
[youtube https://www.youtube.com/watch?v=–klvUya99s?rel=0&showinfo=0&w=560&h=315]
How serious is Raynaud’s?
There are two different types of Raynaud’s: Primary and secondary. Primary Raynaud’s is usually the less serious of the two types, as the condition is mild and manageable; while people experiencing secondary Raynaud’s will usually have more severe symptoms.
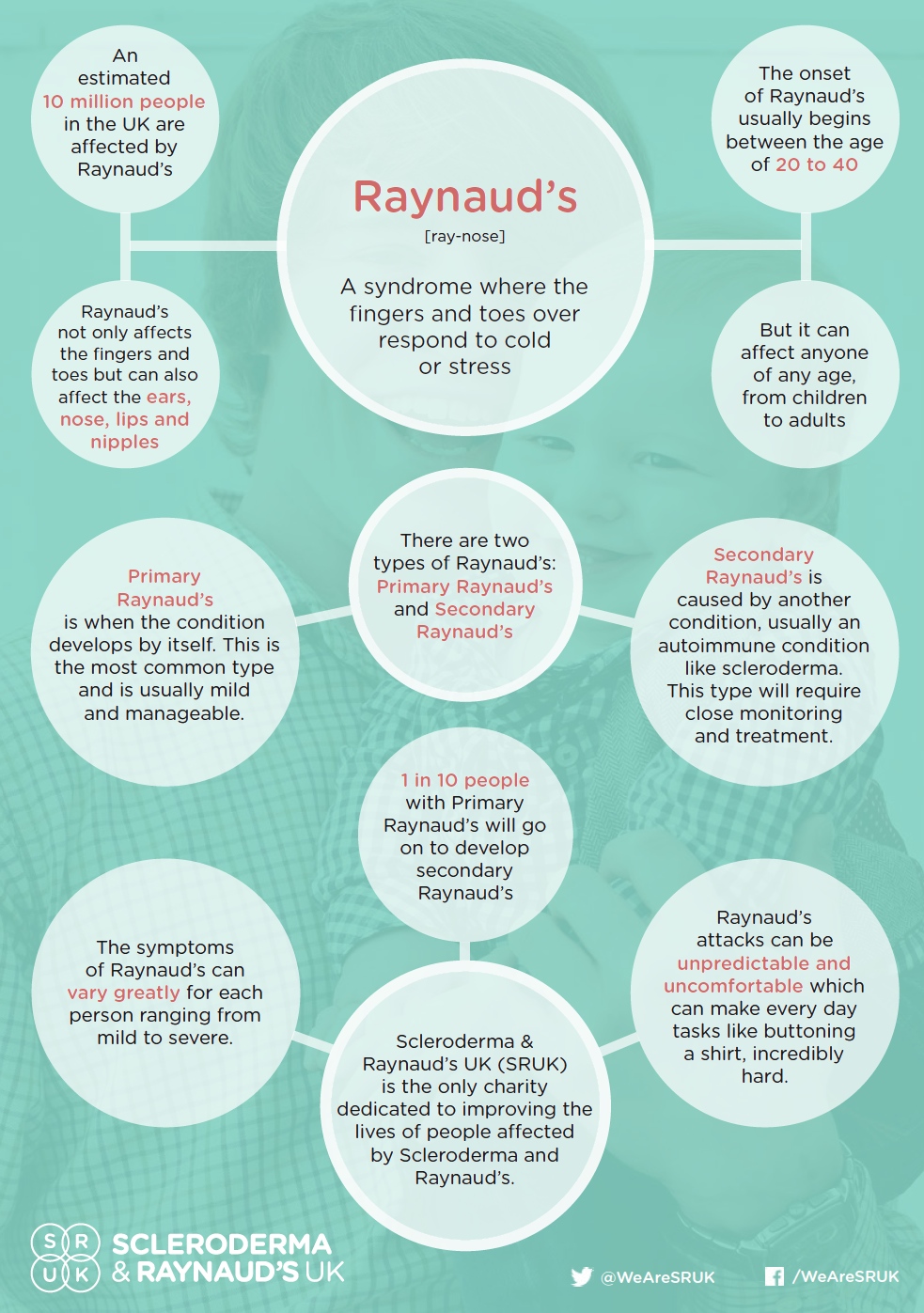 Primary Raynaud’s
Primary Raynaud’s
This is usually mild and manageable and there are ways to help manage the symptoms. People with primary Raynaud’s symptoms tend to have no other complications, and only occasionally go on to develop a related problem. People with primary Raynaud’s should book an appointment with their GP if they are worried about symptoms or if it impacts their life through pain, or if they have any other symptoms, or another health condition.
Secondary Raynaud’s
This is where Raynaud’s is caused by another condition, usually an autoimmune disease like scleroderma or lupus. Secondary Raynaud’s needs more investigation and more careful monitoring for complications like ulceration or sores. People who have noticed a change in their symptoms, are worried about their symptoms, if they have any other symptoms, or another health condition should book an appointment with their GP promptly to ask about Raynaud’s.
[youtube https://www.youtube.com/watch?v=3BUxpfB6nys?rel=0&showinfo=0&w=560&h=315]
If you have any of the symptoms listed, there is a chance that it could be Raynaud’s.
Take SRUK’s online test to find out if you may have the condition. If you do experience these symptoms, then please visit:
www.sruk.co.uk for further information.

Managing Raynaud’s
Although there is no cure for Raynaud’s, it can be managed. The key to managing Raynaud’s symptoms is to try to prevent an attack – hence why planning ahead is vital. Here are some ways you can manage Raynaud’s phenomenon symptoms and live as normal a life as possible.
Keep warm
Do all you can to avoid cold environments, touching cold items or spending time in areas where temperatures fluctuate. Even a slight change in temperature can cause an attack. Wear lots of thin layers and loose clothing in order to remain as warm as possible. Use hand warmers, gloves and thick socks to keep cold fingers and toes comfortable on chilly days.
Relax and pace yourself
Try to steer clear of stressful situations as stress and anxiety can trigger an attack – though that is evidently easier said than done in the busy world in which we live! If possible, try to take rests when you can to avoid getting too fatigued. The Pulmonary Hypertension Association describes a good way of helping to focus on your breathing, called
controlled breathing, (also known as diaphragmatic breathing) which uses your diaphragm and lower chest muscles. Controlled breathing can sometimes help you to switch off from the busy world around you, by focusing entirely on your breathing.
Speak to your doctor about treatments
One medicine, called
Nifedipine, is a calcium channel blocker that is licensed for use in people with Raynaud’s. Nifedipine doesn’t cure Raynaud’s, but it can help to relieve some of the symptoms. Other medications have been used to treat Raynaud’s, with mixed results, including complementary therapies, can be found on SRUK’s
treatments section.
[youtube https://www.youtube.com/watch?v=D-TYmia8VWI?rel=0&showinfo=0&w=560&h=315]
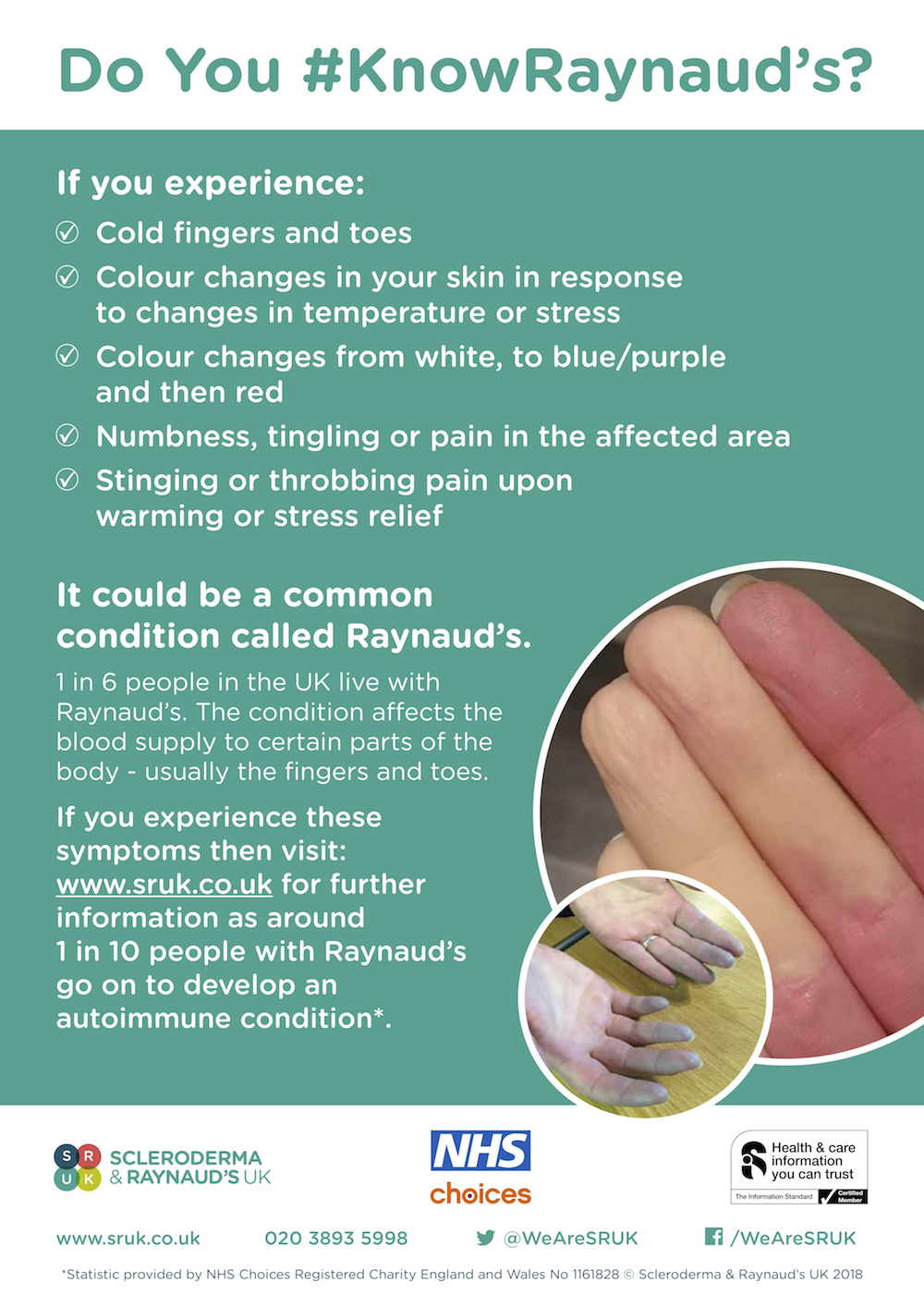
Source: Scleroderma & Raynaud’s UK
 In people who have Raynaud’s, the small blood vessels in the extremities such as the hands, feet, fingers or toes are over-sensitive to even the slightest changes in temperature, the cold and sometimes stress. This causes a Raynaud’s attack where the fingers sometimes change colour, but not always, from white, to blue, to red.
A Raynaud’s attack can be an uncomfortable, and possibly painful, process. It can also make everyday tasks, like buttoning a jacket or unzipping a purse, very difficult. Raynaud’s symptoms generally affect the fingers and toes, but all extremities can be involved, including the hands, feet, ears, nose, lips, tongue and nipples.
In people who have Raynaud’s, the small blood vessels in the extremities such as the hands, feet, fingers or toes are over-sensitive to even the slightest changes in temperature, the cold and sometimes stress. This causes a Raynaud’s attack where the fingers sometimes change colour, but not always, from white, to blue, to red.
A Raynaud’s attack can be an uncomfortable, and possibly painful, process. It can also make everyday tasks, like buttoning a jacket or unzipping a purse, very difficult. Raynaud’s symptoms generally affect the fingers and toes, but all extremities can be involved, including the hands, feet, ears, nose, lips, tongue and nipples.
 Symptoms of Raynaud’s include:
Symptoms of Raynaud’s include:
 Primary Raynaud’s
This is usually mild and manageable and there are ways to help manage the symptoms. People with primary Raynaud’s symptoms tend to have no other complications, and only occasionally go on to develop a related problem. People with primary Raynaud’s should book an appointment with their GP if they are worried about symptoms or if it impacts their life through pain, or if they have any other symptoms, or another health condition.
Secondary Raynaud’s
This is where Raynaud’s is caused by another condition, usually an autoimmune disease like scleroderma or lupus. Secondary Raynaud’s needs more investigation and more careful monitoring for complications like ulceration or sores. People who have noticed a change in their symptoms, are worried about their symptoms, if they have any other symptoms, or another health condition should book an appointment with their GP promptly to ask about Raynaud’s.
[youtube https://www.youtube.com/watch?v=3BUxpfB6nys?rel=0&showinfo=0&w=560&h=315]
If you have any of the symptoms listed, there is a chance that it could be Raynaud’s. Take SRUK’s online test to find out if you may have the condition. If you do experience these symptoms, then please visit: www.sruk.co.uk for further information.
Primary Raynaud’s
This is usually mild and manageable and there are ways to help manage the symptoms. People with primary Raynaud’s symptoms tend to have no other complications, and only occasionally go on to develop a related problem. People with primary Raynaud’s should book an appointment with their GP if they are worried about symptoms or if it impacts their life through pain, or if they have any other symptoms, or another health condition.
Secondary Raynaud’s
This is where Raynaud’s is caused by another condition, usually an autoimmune disease like scleroderma or lupus. Secondary Raynaud’s needs more investigation and more careful monitoring for complications like ulceration or sores. People who have noticed a change in their symptoms, are worried about their symptoms, if they have any other symptoms, or another health condition should book an appointment with their GP promptly to ask about Raynaud’s.
[youtube https://www.youtube.com/watch?v=3BUxpfB6nys?rel=0&showinfo=0&w=560&h=315]
If you have any of the symptoms listed, there is a chance that it could be Raynaud’s. Take SRUK’s online test to find out if you may have the condition. If you do experience these symptoms, then please visit: www.sruk.co.uk for further information.

 Source: Scleroderma & Raynaud’s UK
Source: Scleroderma & Raynaud’s UK
